|
12/7/2023 0 Comments Copd flutter device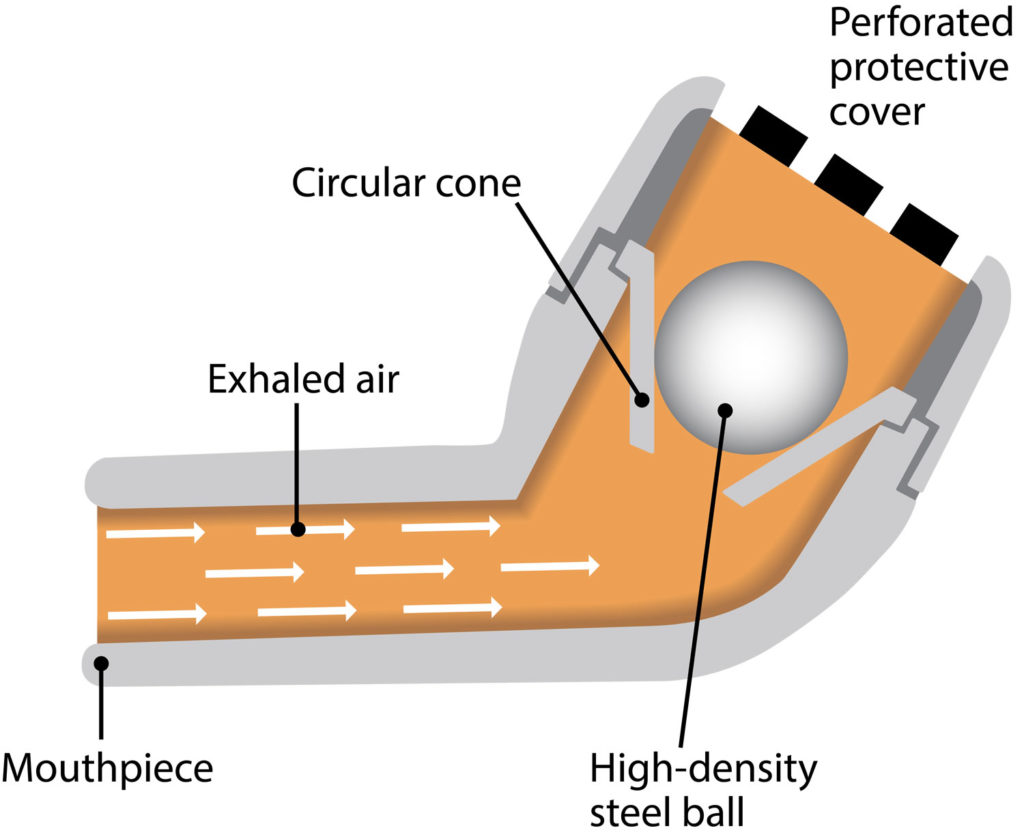
Training on the Flutter® Device and ACBT Physiotherapy MethodĪll patients received basic information and training on bronchiectasis and respiratory physiotherapy on an individual basis. Figure 3 presents the flowchart for the study. Patients were randomized into two separate study groups by a faculty member at the Department of Statistics of University using the MedCalc 11.5.1 package program. Twenty patients in each group, namely the ACBT and Flutter® groups, practiced home-based respiratory physiotherapy while continuing to receive their current treatment regimens. The diagnosis of bronchiectasis was confirmed both clinically and by HRCT. A total of 40 patients, who were diagnosed with bronchiectasis and admitted to the Chest Diseases Department at the University Medical Faculty Hospital between December 2009 and March 2010 were included in this study if they complied with the inclusion criteria and met none of the exclusion criteria. An approval by the Ethics Committee of the Trakya University School of Medicine, protocol no was 2009/153 and registered under the number 12/08, was obtained before commencing the study. The aim of the study was to compare the efficacy of ACBT techniques with the Flutter® device in bronchiectasis patients.Ī prospective, randomized study was conducted to compare Flutter® and ACBT methods in patients with bronchiectasis. To our knowledge, there have not been many trials on evaluating effectiveness of home-based physiotherapy program. Daily use of the Flutter® device at home was as effective as ACBT in patients with non-CF bronchiectasis, and it leads to higher levels of adherence by patients. The positive expiratory pressure was shown to be more effective than Flutter® in terms of preserving pulmonary function, hospital admissions, and antibiotic use in patients, who were followed up for 1 year. A study comparing autogenous drainage with Flutter® reported no differences in the amount of sputum produced by application of either of the two methods however, the Flutter® device was reported to be more effective in reducing viscoelasticity of the secretion. The objective of the present study was to compare the efficacy of home-based respiratory physiotherapy, either by means of the Flutter® device or by ACBT, on symptoms, sputum production, and perception of dyspnea, pulmonary functions, and health-related quality of life in patients with bronchiectasis. 
The flowchart for performing an Active Cycle of Breathing Technique: BC, breathing control TEE, thoracic expansion exercise FET: forced expiration technique ( ) While breathing control prevents or diminishes airway narrowing, thoracic expansion exercises prevent deleterious effects of percussion ( Figure 2). It is flexible, requires patient’s active participation, and requires neither the use of any specific devices nor any specific positioning. Active cycle of breathing techniques (ACBT) is a standard technique, and it bears some advantages. Flutter® is a simple handheld device that allows removal of mucus from the airways using positive expiratory pressure ( Figure 1). In this regard, the Flutter® device represents an alternative to traditional physiotherapeutic modalities and has been increasingly used in the management of respiratory conditions characterized by chronic sputum production. However, these conventional techniques have also been reported to result in temporary adverse effects on physiological parameters during the treatment phase and require the assistance of others. Traditional physiotherapeutic methods used in patients with chronic pulmonary conditions such as bronchiectasis or cystic fibrosis increase the expectorated sputum volume as well as alveolar ventilation and decrease the frequency of infections. The objectives of treatment include achieving symptom control, preventing or reducing exacerbations, decelerating the progression of pulmonary injury, maintaining airway patency, and improving the quality of life, all of which are the factors to be accomplished merely by decreasing bronchial infection and inflammation and by increasing the mucociliary clearance. There are no definitive treatments of bronchiectasis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
